
How Trauma Rewires the Brain — and How You Can Rewire It Back with CBT Techniques
Introduction: Trauma Changes the Brain — But Change Is Not Permanent
Trauma is often misunderstood as a purely emotional experience or a “lack of mental toughness.” In reality, trauma is a physiological event that lives in the brain, the body, and the autonomic nervous system. If you’ve ever wondered why you overreact to small stressors, struggle to find a sense of “calm,” replay painful memories against your will, or feel stuck in patterns you logically know aren’t helpful—there is nothing wrong with you.
Your brain adapted.
When we experience a traumatic event—or a series of prolonged stressful events—the brain undergoes a structural and functional shift. It literally rewires its circuitry to prioritize survival over safety and protection over presence. This survival-based wiring is the root of nervous system dysregulation, a state where your internal “alarm” is stuck in the “ON” position long after the threat has passed. This isn’t a sign of weakness; it is a biological achievement. Your brain successfully learned how to keep you alive during a period of peril.
To understand the physiological side of this state, explore our guide: 👉 The Path Out of Survival Mode: Tools to Calm an Overactive Nervous System
The good news is that the human brain possesses neuroplasticity. The same mechanism that allowed trauma to reshape your neural pathways also allows healing to reshape them back. With the right tools—specifically Cognitive Behavioral Therapy (CBT) and nervous system regulation—you can retrain your brain to feel safer, calmer, and more in control. These foundational principles are introduced in: 👉 CBT Mindset: Happiness, Growth, and Personal Transformation
What Trauma Actually Does to the Brain: The Anatomy of Survival
Trauma is not defined by the event itself, but by how the nervous system processes it. When a situation overwhelms your ability to cope, the brain’s “operating system” shifts from the higher-level “Thinking Brain” to the lower-level “Survival Brain.” This shift alters how three key regions function and communicate.
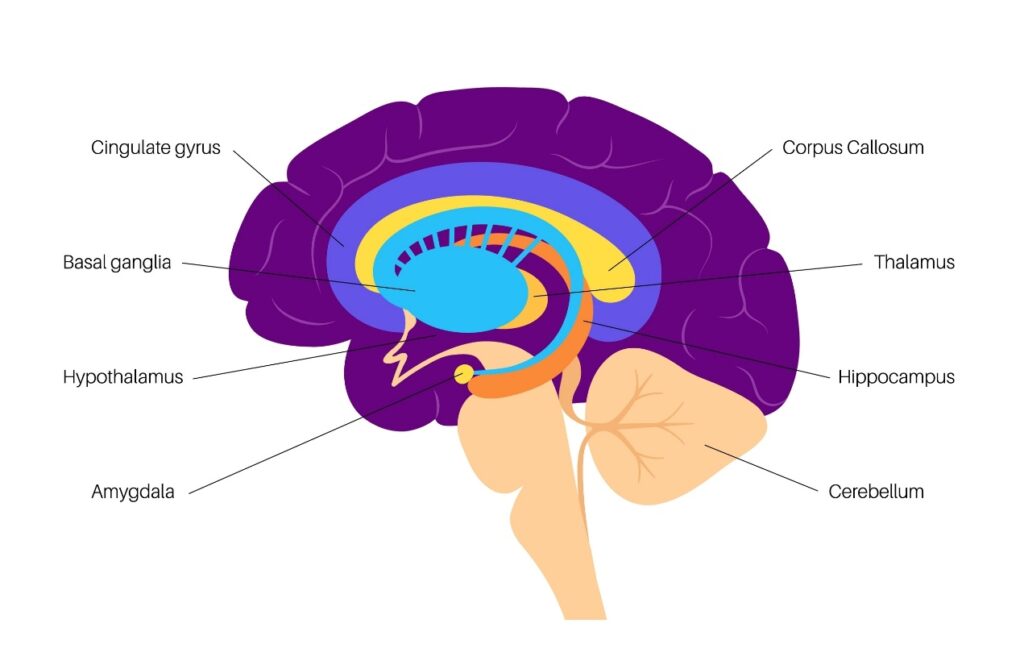
1. The Amygdala: The Hyperactive Smoke Detector
The amygdala is the brain’s threat detector. Its job is to scan the environment for danger and trigger the “fight-or-flight” response. In a brain impacted by trauma, the amygdala becomes hyper-responsive. It no longer distinguishes between a looming work deadline and a physical predator.
- Hypervigilance: Your brain is constantly “scanning” for what might go wrong.
- Panic: Sudden bursts of adrenaline and cortisol without an obvious trigger.
- Emotional Reactivity: You might find yourself snapping at a loved one or crying over a minor inconvenience because your amygdala perceives these events as existential threats.
The National Institute of Mental Health (NIMH) notes that this hyperactivity keeps the body in a state of high-alert, making it nearly impossible to rest. 👉 NIMH – Post-Traumatic Stress Disorder (PTSD)
2. The Prefrontal Cortex: The Offline CEO
The prefrontal cortex (PFC) is responsible for logic, planning, and impulse control. It is the “Executive” of the brain. When trauma occurs, the connection between the PFC and the amygdala is weakened. In the heat of a trigger, the “logical” part of your brain effectively goes offline.
- Decreased Rationality: This is why you cannot “reason” yourself out of a panic attack.
- Difficulty Focusing: Because the brain is prioritizing survival, it diverts energy away from the PFC, leading to “brain fog” or trouble concentrating on tasks.
CBT techniques are designed to strengthen this “logical” muscle, eventually allowing it to exert better control over the emotional center. 👉 Mindfulness & Managing Thoughts: Decentering with CBT
3. The Hippocampus: The Disorganized Librarian
The hippocampus is responsible for memory consolidation. It places a “date and time” stamp on memories, filing them away in the past. Trauma, however, causes the hippocampus to lose efficiency (and in chronic cases, even shrink).
- Blurred Time Perception: The brain cannot tell that the traumatic event is over. It feels like it is happening right now.
- Flashbacks: Because the memory isn’t “filed” properly, it remains “live,” easily triggered by smells, sounds, or sensations.
Research via the NIH confirms that chronic stress reduces hippocampal volume, but also shows that this volume can be restored through healing and regulation. 👉 NIH – Stress, the Hippocampus, and Memory
Why Trauma Keeps You Stuck: The Four Survival Responses
Trauma trains the brain to stop asking “What brings me joy?” and instead ask, “How do I stay safe?” When the brain is focused on survival, it falls into one of four primary patterns. Understanding yours is the first step toward using CBTeffectively.
Image showing the 4 survival responses: Fight, Flight, Freeze, and Fawn
- Fight (The Protective Aggressor): This isn’t just physical fighting. It manifests as a need for control, perfectionism, chronic irritability, and a “me-against-the-world” mentality.
- Flight (The Anxious Overachiever): This manifests as “workaholism,” constant busyness, anxiety, and an inability to sit still. If you stop moving, you feel the “dread” catch up to you.
- Freeze (The Numb Avoidant): This is characterized by dissociation, feeling “spaced out,” procrastination, and physical heaviness. The brain decides the best way to survive is to “play dead.”
- Fawn (The People-Pleaser): This involves self-abandonment to appease a potential source of danger. You become hyper-attuned to other people’s moods and sacrifice your own needs to maintain “peace.”
These patterns are explored through a CBT lens in: 👉 CBT & Authentic Expression: Balancing Your Inner and Outer Self
Neuroplasticity: The Science of Hope
For decades, we believed the brain was “fixed” after childhood. We now know that the brain is like plastic—malleable and capable of change at any age.
Imagine your brain is a field of tall grass. Trauma is like a truck that drove over the grass thousands of times, creating a deep, muddy rut. Whenever a thought enters your head, it naturally falls into that rut. Healing is the act of intentionally walking a new path.
Initially, walking through the tall grass is exhausting and slow. But with every repetition of a CBT exercise or a grounding technique, the grass is matted down. Eventually, the “safety path” becomes easier to walk than the “trauma rut.” The American Psychological Association (APA) confirms that these behavioral changes lead to physical rewiring. 👉APA – Neuroplasticity and the Brain’s Ability to Change
How CBT Helps Rewire the Brain: A Step-by-Step Guide
Cognitive Behavioral Therapy (CBT) targets the CBT Triangle: the interconnected relationship between our Thoughts, Emotions, and Behaviors. By changing one, we eventually shift the others.
Phase 1: Identifying Trauma-Based Core Beliefs
Trauma installs “Core Beliefs”—the “operating rules” of your life. These are often rigid and extreme. Common trauma-based core beliefs include:
- “I am fundamentally broken.”
- “The world is a dangerous place.”
- “I cannot trust myself to handle intense emotions.”
The CBT Intervention: Use a “Downward Arrow” technique. Ask yourself, “If this thought were true, what would it mean about me?” until you find the core belief. Once identified, we don’t just “think positive.” We look for evidence.
- Exercise: Write your core belief on one side of a paper. On the other, list three times in the last week where that belief was not 100% true.
Phase 2: Cognitive Restructuring (The Thought Audit)
In survival mode, the brain uses Cognitive Distortions—mental filters that amplify threat.
- Catastrophizing: “If I don’t answer this text perfectly, they will leave me and I’ll be alone forever.”
- All-or-Nothing Thinking: “If I’m not perfect, I’m a failure.”
The CBT Tool: The Thought Audit
- Step 1: Write the automatic survival thought.
- Step 2: Identify the distortion.
- Step 3: Generate a “Balanced Perspective.”
- Reframe: “I am feeling anxious about this text because I value the relationship. One text does not determine my entire future.”
Templates are available here: 👉 Free Downloadable CBT Tools
Phase 3: Behavioral Experiments and Exposure
The amygdala only learns through experience, not through talking. Trauma teaches us that the only way to be safe is to avoid. CBT teaches “Safe, Gradual Exposure.”
- The Experiment: If you fear social settings, a behavioral experiment might be going to a coffee shop for 10 minutes.
- The Goal: You prove to your amygdala that you can enter a “trigger” zone, feel the discomfort, and survive. This provides a Corrective Experience that physically rewires the amygdala’s sensitivity.
Explore different therapy modalities that support this: 👉 Types of Therapy: CBT, DBT, EMDR, and More
Rewiring the Filter: Retraining the RAS
The Reticular Activating System (RAS) is a bundle of nerves at the brainstem that acts as a gatekeeper. It decides what information is worth your attention. In survival mode, your RAS is programmed to find “Threats.” It will ignore 99 kind gestures and fixate on one judgmental look.
The “Glimmer” Practice
To rewire the RAS, we must consciously look for Glimmers—micro-moments of safety, beauty, or connection.
- The warmth of the sun on your skin.
- A funny meme that made you chuckle.
- The feeling of a clean bedsheet.
The Exercise: Every night for 30 days, write down three glimmers. This “programs” your RAS to look for safety cues the next day. Over time, your brain begins to filter for safety as naturally as it once filtered for danger.
Restoring the Sleep-Safety Connection
Trauma often disrupts sleep because the brain views sleep as a time of extreme vulnerability. If your “smoke detector” is on, it will wake you up at 3:00 AM to scan the room.
The Cognitive Offload
To help your brain go “off-duty,” you must “park” your survival thoughts before bed.
- Write down your “Threat List”: Everything you are worried about for tomorrow.
- Assign a “Safety Action”: Beside each item, write one small thing you can do (or a statement like, “I have handled this before”).
- Physical Closure: Close the notebook. This physical act tells the brain the “shift” is over.
Cognitive Shuffling
Use “Cognitive Shuffling” to occupy the threat-scanner. Think of a word (e.g., “CALM”). For C, visualize as many neutral objects as possible (Cat, Car, Cake). Then move to A. This prevents the brain from entering the “threat-loop” as you fall asleep.
Why CBT Works Best with Nervous System Regulation
One of the most important lessons in trauma recovery is: You cannot reason with a brain that thinks it is dying.
If your heart is racing and your breath is shallow, your prefrontal cortex is offline. Trying to do CBT “reframing” during a panic attack is like trying to fix a computer while the building is on fire. You must put out the fire first.
The “Bottom-Up” Strategy:
- Regulate (Body First): Use 4-8 breathing, splash cold water on your face, or do “Wall Pushes.” This tells the brainstem, “The environment is safe.”
- Relate (Emotions): Acknowledge the feeling. “I am feeling a survival response. It is my body trying to protect me.”
- Reason (Mind): Once your heart rate slows, then use CBT to reframe the thought.
This integrated approach is the foundation of our work: 👉 Emotional Intelligence (EQ) & CBT Training
The Role of Self-Compassion as a Biological Tool
Many trauma survivors try to “shame” themselves into being better. They say, “Why can’t I just get over this?” or “I’m being so weak.”
Biologically, shame is a threat. When you criticize yourself, you activate the amygdala, keeping yourself in survival mode. Self-compassion is not a “soft” luxury; it is a clinical necessity for rewiring. By treating yourself with the same kindness you would show a wounded friend, you provide the “Felt Safety” required for neuroplasticity to occur.
Frequently Asked Questions (FAQs)
Q: How long does it take to see changes in my brain?
A: Neuroplasticity is a marathon, not a sprint. While some people feel a “lightness” after a few sessions, structural changes in the brain (like shrinking the amygdala’s reactivity) typically take 8 to 12 weeks of consistent practice.
Q: Can I heal if my trauma happened decades ago?
A: Yes. Because neuroplasticity exists throughout the lifespan, it is never too late to rewire your brain. Your brain is always responding to the current input you give it.
Q: Does rewiring mean I will forget what happened?
A: No. Healing isn’t about erasing the memory; it’s about changing the charge of the memory. A rewired brain remembers the past as a “story” rather than a “current emergency.”
Final Thoughts: You Are Not Broken
Your brain adapted to protect you. That adaptation kept you alive during your most difficult moments. It was a brilliant, necessary strategy at the time. But now, those same survival mechanisms are preventing you from living the life you deserve.
Exiting survival mode is a journey of reclaiming your body from your past. Through CBT, nervous system regulation, and compassionate repetition, your brain can learn that the “war” is over. You are no longer in danger. You have choice. You can heal.
Ready to start your journey? Explore our Blog Articles or join the Better Mind Club Academy today.
